News
Pass the scalpel: Mid-level surgical staff save lives in Ethiopia
- 14 July 2015
News
AMHARA REGION, Ethiopia – Harsh fluorescent lights, fading paint and cracked chairs greet visitors at the Finote Selam District Hospital, in Ethiopia’s remote Amhara Region. But despite its humble appearance, this hospital is a game changer. Without expensive upgrades or expansions, it has dramatically increased the care it provides to pregnant women – and the lives it saves.
“Many could have died if we were not here,” said Kebede Seid.
Mr. Kebede is one of three emergency surgical officers at the hospital, deployed there three years ago as part of a ‘task-shifting’ programme, which teaches emergency surgical and obstetric skills – such as performing a Caesarean section – to mid-level health professionals. Such tasks had previously been reserved only for doctors.

Today, the hospital can handle a wide range of pregnancy and labour complications. As a result, it sends fewer women away to seek care at better-equipped, but faraway, facilities.
“If we did not do Caesarean sections, we would have seen many mothers dying en route to referral hospitals,” Mr. Kebede said.
The country’s task-shifting initiative began in 2009 to address an acute shortage of health workers. Three universities, working with the health and education ministries and UNFPA, began offering a three-year graduate programme for health professionals, equipping them with the skills to handle life-threatening maternal health problems.
Finote Selam District Hospital is one of many district hospitals to receive the graduates, known as emergency surgical officers. Their skills have greatly increased the services available, attracting more women to the hospital for care.
Two years ago, the hospital performed 50 to 60 deliveries a month. Now the hospital delivers 115 to 120 babies each month – and sometimes as many as 170.
Many patients suffer pregnancy complications, which are referred from health centres in the nine surrounding ‘woredas,’ or districts. Women also come from as far as 100 km away to seek care. Cases often involve hypertension, antenatal or post-partum haemorrhage, obstructed labour, complications of abortion, or infection.
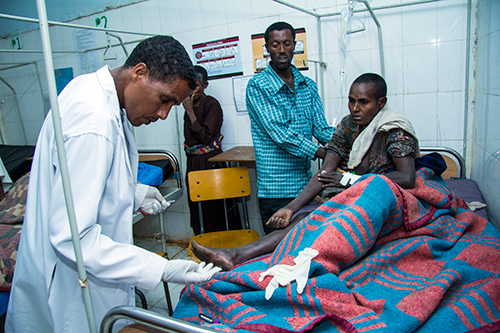
“All are dangerous to the life of the mother,” Mr. Kebede noted.
Referrals to the hospital are increasing all the time. Still, experts believe many more women should receive emergency maternal care. The problem is that many health centres are unsure when send women to the hospital.
“They do not know who to refer and when,” said Mr. Kebede. There are also dangerous delays in referring women to emergency care. “They do not decide fast,” he said.
In the past two and a half years, the Finote Selam District Hospital saw only two maternal deaths – a major change from the prior years. One woman suffered from eclampsia and died on arrival. Another had sepsis when she arrived, and died shortly after delivering.
Both could have survived, Mr. Kebede noted, if they had arrived earlier.
Currently, 11 universities and 33 affiliate hospitals are implementing the task-shifting programme. There is an average enrolment of 175 students a year, and the programme aims to train 800 to 1,000 health workers by 2020.
The Government plans to deploy at least one emergency surgical officer in each district hospitals in the country.
The success of the programme has prompted further improvements, as well. The number of emergency surgical officers is so great, facilities are now being expanded and upgraded to accommodate them.
This will help address the health system’s dilapidated infrastructure. “In some places, they have the beds but not the room,” Mr. Kebede explained. “Some woredas have turned waiting rooms to warehouses.”