News
Getting help to nomad moms on the move in West Darfur
- 12 July 2016
News
WEST DARFUR, Sudan – Something was terribly wrong. Zahra Zakaria was eight months pregnant when she went into labour in a tent in Kondabi, a remote village in Sudan’s West Darfur state. It was her sixth childbirth, but the pain this time was different.
“Unlike my previous five deliveries, I felt pains from complications this time,” she later recalled. She was suffering from an obstructed labour – a potentially deadly condition.
Ms. Zakaria, 32, belongs to a nomadic community in West Darfur. She and her family move continuously in search of water and pasture for their cattle. Like many nomad women, she had never visited a health facility or been seen by a midwife.
When it became apparent that she could not deliver on her own, her family called for a traditional birth attendant, someone who customarily assists during childbirth but who has no formal medical training.
The birth attendant was unable to help, leaving Ms. Zakaria in agony for two full days as her labour failed to progress.
Sudan has high rates of pregnancy-related mortality. A Sudanese woman has a one in 71 risk of dying from maternal causes in her lifetime, according to a recent joint UN publication.
In West Darfur, the risks are worse. The state has the second highest maternal death rate in the country, according to a 2010 survey. And among vulnerable groups like Ms. Zaharia’s community, the dangers are even greater.
There are an estimated 75,000 nomads in West Darfur. Their travels take them far from health facilities, and nomadic women often perform arduous tasks throughout their pregnancies, such as following herds into the pasture for long hours.
Ms. Zakaria’s own health had been an afterthought while she was pregnant – until the delivery nearly killed her.
On her third day of labour, her family finally managed to find a trained midwife, who urged them to bring her to a hospital immediately. The nearest hospital was at Elgeneina, the state capital, which required them to find a car for transport. It ended up costing them 400 Sudanese pounds.
“This amount of money is not a joke for us,” said a family member, “but we managed to collect it.”
Ms. Zakaria arrived in the dead of night, accompanied by her husband and father.
Fortunately, the hospital was able to manage complications like hers. In 2014, its maternity ward was thoroughly rehabilitated with help from UNFPA and the United States Agency for International Development.
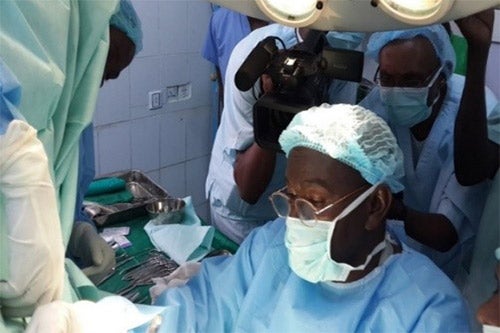
A Caesarean section was quickly performed, saving Ms. Zakaria’s life and that of her baby boy.
Before the hospital was rehabilitated, it had only one delivery room and five beds, and there was a single, poorly stocked operating theatre.
Today, there are four delivery rooms and 50 beds, as well as two well equipped operating theatres. The hospital now conducts 60 to 70 Caesarean sections per month, in addition to 110 to 140 vaginal deliveries.
The upgrades have “improved the capacity and quality of the services [and] maintained the dignity of women,” said Dr. Alaa Eldeen, a senior gynaecologist at the hospital.
When asked why she had not received antenatal care, Ms. Zakaria joked, “The herd owner is crazy.” She – along with her family – is the owner of her herd. It was a way of reflecting on how little concern she had given to her own well-being.
UNFPA is now working with midwives to reach these communities, helping them to prioritize women’s health.
A yearlong training programme at the midwifery school in Elgeneina is supported by UNFPA. In each class, five midwives come from nomadic groups. Upon graduation, they will move with their communities, providing essential health services.
UNFPA is also planning an awareness campaign about the importance of receiving antenatal care, safe delivery services and other reproductive health care. As part of this campaign, trained midwives will spread messages about maternal health and family planning, and help direct women to further health care.