News
Delivering Hope to Women with Fistula in Niger
- 25 September 2007
News
NIAMEY, Niger — Fifty-five-year-old Hanna Moussa keeps a carefully wrapped bar of soap with her at all times. She’s saving the soap for her grandson, who helped care for her when she was shunned by most of her family because of a fistula injury, which caused her to leak urine uncontrollably.
“I’m keeping it for my grandson to thank him for taking care of me,” she explains.

Obstetric fistula is a preventable childbirth injury that can, as in Hanna’s case, cause chronic incontinence, leaving sufferers stigmatized by their families and communities. Without treatment, they may become social outcasts.
“It’s a shame for the family,” says Nafissatou Imorou, who translated Hanna’s story. “They isolated her in a corner of the (family) compound. They think she is bad luck.”
Fistula occurs when a woman endures obstructed labour for days on end without medical intervention, usually a Caesarean section. In most cases, the baby dies. Of the ten pregnancies Hanna carried, eight of her children were stillborn or died before they reached five months of age, resulting in her husband abandoning her. “My husband doesn’t exist for me anymore,” she says.
Reconstructive surgery can usually mend the injury, but most women cannot access or afford medical treatment. Hanna was more fortunate than most, receiving treatment and a temporary home from Dimol, an NGO dedicated to the prevention, treatment and reintegration of fistula patients. It is supported by UNFPA, the United Nations Population Fund.
"They isolated her in a corner of the (family) compound. They think she is bad luck. "
“Fistula is something we could avoid if (women) have access to emergency obstetric care,” said Issa Sadou, the programme officer in charge of Gender and Fistula in the UNFPA Niger office. “That’s why we work with NGOs and hospitals – to put the emphasis on prevention.”
Dimol’s Director, Salamatou Traoré says healing a fistula patient is not simply a case of treating her physical injuries.
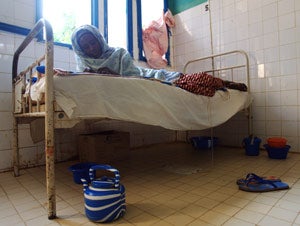
“To cure a woman, you must first treat her psychologically: You make her at ease with other women. She needs to socialize with other women especially if she has been isolated,” she says. “(At Dimol) she is given a sheet, and bed and realizes her value. She cooks with other women. She is given two cakes of soap to take care of her hygiene.”
Hanna comes from Dantidi, 700 km east of Niamey and a day’s journey away. She found out about Dimol, which means ‘dignity’ in the Peulh language, through a community sensitization campaign.
Public service announcements publicizing the arrival of surgical teams to Niamey are broadcast throughout the country on community and national radio stations in five local languages. “They publicize when a surgical team is arriving, “ says Sadou. “Then the women come en masse.”
There are many reasons for the high rates of fistula in Niger. Early marriage is endemic here sometimes by girls as young as 11 years old. Many women and girls may be reluctant to be seen by a male health care worker. Others may not seek treatment because their family won’t allow it.
“She can’t decide herself to come to the hospital because of family pressure,” Sadou said. “Her parents might refuse to listen to her when the contractions are underway. Traditionally, she must not show the pain, and her babies die, and she is injured.”
Traoré can tell how many days a woman has been in labour by the extent of her injuries. “The longer they labour without assistance, the more they are injured. Some can barely walk because of nerve damage.”
Traoré recalls the recent case of a 15-year-old girl from the village of Foneko, about 25 kilometres west of Niamey. “She hid herself in a field of millet so that no one would see her, because she was ashamed,” she recounts. “We searched high and low for her through the gardens and throughout the village. Finally a man spotted her. Now she’s in the hospital.”
In 2006, the Government of Niger decided to make Caesarean sections free of charge to any woman who needed them as part of an effort to stem the number of fistula cases and the rate of maternal mortality in Niger, among the highest in the world. For every 100,000 live births, 700 women die, according to the Ministry of Health. Only 16 per cent of women give birth in the care of a trained attendant.
“We are trying to protect women and children,” said Niger Health Minister Mahamane Kabaou. “We know many women are losing their lives giving life. We want women not to suffer giving life, and now all Caesareans are free.”
Even with free treatment, qualified medical expertise is in short supply. Niger has a population of 13 million people, and only six doctors are operating on fistula cases in the country. Few doctors are interested in treating fistula cases, said Dr. Idrissa Abdoulaye, a surgeon conducting fistula repair at Niamey’s National Hospital.
“If I leave them it would be a betrayal. I would like to try to interest other surgeons (in treating fistula), but it’s hard to find someone,” Dr. Abdoulaye said. “These poor women – we must give them aid. It is a vocation.”
Many have difficulty accessing urban areas where treatment can be obtained either because of cost or lack of transport.

“Public transport refuses to take them, because they smell, and they don’t want them urinating in the bus,” Traoré says. “The women themselves are often afraid they will urinate in the bus on their way to the centre.”
Dimol has developed its own protective clothing. Originally, it was made of plastic, which proved too hot in Niger’s stifling climate. Now they buy cotton panties in the market, which they line with blue plastic. A washable sponge is fastened in the middle to collect leaking urine.
Treating a fistula patient in Niger costs approximately $300, which includes the three to four months she stays in Dimol waiting to be operated on and during her recovery. Each woman returning to her village receives 50,000 CFA, or about $100, for income-generating activities, which help her reintegrate into her community.
“We take the women who have already been cured from village to village, and they bear witness to what they have suffered and how they have been treated. …They are a living witness of what they have been through,” Traoré says. “That way we can make sure there are no more cases. We need to continue sensitization. It’s important to show what they’ve been through. Sometimes the women cry that hear their stories. We sensitize their husbands, families and communities.”
Twenty-six-year-old Salamatou Aouzeidi traveled 600 kilometres from her mountain village to get to Dimol in Niamey. It took three operations to fully repair her, and she’s eager to go home.
“When I return there will be a big party, now that I am cured,” she says.
Hanna still leaks urine when she lies down, and despite considerable progress during her two-year convalescence, she is considered an incurable case. “I’m happy, because I can walk again and get around. But I think always of home,” she says.
Sadou said UNFPA would work with the NGO to negotiate with Hanna’s family to take her back. “We want fistula to be considered not as a result of witchcraft, but as any other disease, like malaria, so families won’t reject them,” he says.
— Angela Walker