News
Afghan NGOs Provide Maternal Care Despite Shortage of Skilled Staff
- 19 February 2002
News
KABUL, AFGHANISTAN -- A severe shortage of trained female doctors and midwives is a major obstacle to extending reproductive health care to Afghan women. The vast majority have no access to family planning, prenatal care or assisted deliveries.

The United Nations Population Fund (UNFPA) is working to alleviate the shortage as part of its ongoing assistance to several non-governmental groups that provide health services.
The Swedish Committee for Afghanistan manages a network of over 200 basic health centres and 57 clinics in 6 of the country’s 31 provinces; 24 clinics provide maternal and child health (MCH) services, 14 of them in Kabul.
Women come to the clinics for family planning, prenatal checkups and treatment of reproductive tract infections. Some deliveries are done there, but most women deliver at home. Where possible, patients with complications are referred to emergency obstetric care centres. Health education classes cover family planning methods, child health and the benefits of child spacing.
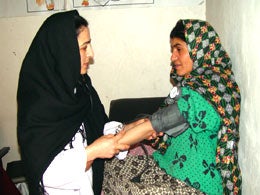
“We would like to extend these services to more clinics,” says Dr. Mohammed Hassan, the agency’s health manager, “but that depends on the availability of qualified female health workers. These are difficult to find in Afghanistan.” The labour shortage reflects a training gap--largely due to the Taliban’s ban on educating women--but also to low salaries and a lack of suitable accommodation and transport in rural areas.
At the Swedish Committee’s small Mirbachacot clinic on the outskirts of Kabul, obstetrician-gynaecologist Dr. Shafiqa examines maternal and child health patients six mornings a week. She also delivers babies, and when necessary refers complications to a maternity hospital. One patient from out of town was saved recently after a traditional birth attendant (TBA) spotted trouble and sent her to the clinic, which referred her to a hospital. But a lack of transport from the countryside delayed her journey, and the baby died.
The Afghan Red Crescent Society operates eight maternal and child health clinics in Kabul, 48 in major cities throughout Afghanistan, according to Dr. Khalid Sharifi, the Society’s regional health officer.
At a typical clinic, nurse-midwives:
Dr. Fatima Nasir supervises the Society’s maternal and child health activities throughout the country, which are supported by UNFPA. After a successful pilot project in 1997, she notes, the agency decided to expand MCH services to all facilities with female staff, to combat extremely high rates of maternal, infant and under-5 mortality.
The effort was made difficult by the shortage of qualified female staff. “We couldn’t find many midwives willing to work in the rural clinics and supervise the local birth attendants,” she says.
UNFPA supports training for midwives, conducted in Peshawar, Pakistan. The midwives, in turn, train TBAs to work in rural communities, conducting prenatal and post-natal exams, assisting deliveries and providing health education.
The UNFPA-supported TBA programme offers 21-day training sessions for birth attendants followed by periodic workshops. Refresher training is also provided for doctors, nurses, midwives and health educators.
“Before we trained the TBAs, most breach patients died during delivery. Most TBAs didn’t know the danger signs of cases requiring referral. The training programme has reduced maternal and infant mortality rates.”

The training programme was developed during the Taliban’s rule. Dr. Nasir says that despite restrictions on travel by women, she was able to visit project sites mostly without interference. Initial limits on women’s freedom to go to clinics were eventually lifted. But only women health workers could examine female patients.
That wasn’t a big problem at one Red Crescent clinic, which had only one male staff member, lab technician Safiullah. Whenever the religious police came to inspect, he had to hide in a bathroom, Dr. Fatima recalls, laughing.
Dr. Jean Gilardi, Afghanistan health coordinator for the International Federation of Red Cross and Red Crescent Societies, underscores the urgent need for more trained female health professionals. “If we can find qualified women doctors and midwives, we will train them as TBA trainers and put maternal and child health in all our clinics. UNFPA’s support in this effort is essential.”
Equally critical, she adds, are the medical supplies the Population Fund provides to the Swedish Committee. These include a variety of family planning methods, other medical supplies and equipment like examination tables and stethoscopes. “The whole range of reproductive health kits is badly needed, including TBA kits and clean delivery kits. These have been very helpful in saving Afghan women’s lives.”
Contact Information:
William A. Ryan
Tel.: +66 2 288 2446
Email: ryanw@unfpa.org