News
Scaling Up Access to Family Planning in Southern Ethiopia
- 11 January 2010
News
WOLAITA SODO, Ethiopia — It’s no ordinary day for Fanaye Fanta.
Since her initial training to become a health extension worker three years ago, Fanaye has taken clients’ temperature and blood pressure and provided information, counselling, condoms and pills.
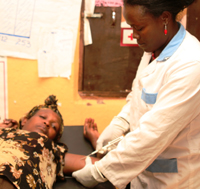
But this is the first time she has inserted a slim plastic rod (Implanon), which serves as a long-acting contraceptive, into a woman’s arm.
Proper placement is critical: If the rod is inserted too deeply it can be difficult or impossible to remove later on. If it is incorrectly inserted and falls out, the woman will not be protected from unintended pregnancy.
Fanaye learned the procedure as part of a five-day training given by the Wolaita Zone Health Department with the support of UNFPA, the United Nations Population Fund. The training is part of the Government of Ethiopia’s comprehensive plan to make Implanon, an effective, long-acting and reversible contraceptive, widely available throughout the country to women who want to delay pregnancy.
Fanaye and 12 colleagues received the training from a nurse supervisor at the Bosa Kacha Health Post, which provides primary health care for communities to the south of Sodo, the capital of the Wolaita Zone in the Southern Region of Ethiopia. The health extension workers have a big task ahead – the new family planning method is expected to be very popular in the Wolaita Zone, one of the most densely populated areas in the country. Early indications show that Implanon, which releases a hormone that prevents ovulation for up to three years, will increase demand for family planning.
The initiative is also part of a larger effort to ‘task-shift’ some health services to less intensively trained health workers in a country where doctors and nurses are scarce. Fanaye is among the 15,000 health extension workers that the Ministry of Health ultimately plans to train for the Implanon country-wide scale up at the kebele (the smallest administrative unit) level.
Once the health extension workers implant the plastic rod, the mother will be given an informational card that she will be advised to keep for future reference. The card is useful for follow-up and removal when the client requests it. Pre-and post-insertion counselling is given to the mothers getting the service. The referral system has been organized in such a way that one nurse supervisor who is based at a Health Centre monitors and evaluates the work of five health extension workers in five Health Posts.
Fanaye needs to successfully insert four more of the Implanon rods before she is certified to conduct them on her own when she goes back to her Health Post. Beaming with enthusiasm she says “the training has given me essential skills and I will be ready to do the insertion on my own when I am done with the training here.” Indeed she articulately describes the steps in the procedure, including pre-and post-insertion counseling.
The enthusiasm and eagerness of Fanaye is shared by her other colleagues who are drawn from different Health Posts and deployed at the Bosa Kacha Kebele Heath Post for the training. They were attentively listening to the nurse supervisor giving them the training. Between them they did nine insertions for the day and were eagerly waiting for more clients.
The mothers seem enthusiastic as well: One mother in line on the first day of the campaign had already borne ten children. Having so many pregnancies is risky in Ethiopia, where maternal mortality is high and increases with each child. According

to the most recent estimates and findings only 6 per cent of pregnant women in Ethiopia have access to professional assistance during pregnancy and child birth, the lifetime risk for dying in pregnancy or childbirth is 1 in 27, compared to 1 in 17,000 in Sweden.
Longer-acting contraceptives can also make it easier for couples to break out of poverty. "My husband and I work on a small plot of land as farmers and we hardly make ends meet to support the family,” said one woman in line to receive an implant. “We have decided that we don't want any more kids and raise what we have. I was using injectables before which have a three months protection. Now that Implanon is available I have switched to it."
The scale-up initiative has gotten off to a good start in the Wolaita Zone. Five-day training was given to a total of 104 health extension workers in mid-December from 14 Health Posts in six woredas (districts) in the zone. In three days, a total of 386 insertions were made, representing over 60 per cent of the target.
Building momentum, however, will require careful planning, logistics and follow-up. While the supplies of Implanon in the zone are adequate, according to Tarekegn Gebremeskel, a Health Officer in the Wolaita Zone, it’s also important to ensure that additional supplies that may be needed, including iodine, supplementary iron and lidocain, are also available.
Also, even a five-day intensive training is not enough to ensure quality of care, an important consideration. Post-training assessments and follow-up monitoring are important to ensure that women are getting correct information and counseling. And referral mechanisms must be in place to deal with possible side effects or removals, which are now being carried out by the nurse supervisors.
- by Abraham Gelaw/UNFPA Ethiopia
Scaling Up the Efforts to Expand Contraceptive Prevalence and Reduce Unmet NeedThe Government of Ethiopia’s comprehensive plan for Implanon initially targets 32 selected woredas (districts) representing 4 per cent of the total in the country. Ethiopia’s Ministry of Health and partners, including UNFPA, have put in more than $12 million into the purchase of supplies and implementation activities. This initial effort will help to identify challenges and recommend remedies. After this first wave will come an evaluation which will allow the Government to recalibrate the implementation before taking it country-wide. The idea is to expand voluntary access to this long-acting family planning method in a country where the unmet need for contraception is quite high. It is believed that giving women access to Implanon as long-term method at the community level will help improve the contraceptive prevalence rate and reduce unmet needs, which are both MDG indicators of maternal health. Ethiopian women have, on average, more that five children, but more than a third say they would like to avoid or delay pregnancy, according to the Demographic and Health Survey (2005). If all currently married women who say they want to space or limit the number children were to use family planning, the contraceptive prevalence rate in Ethiopia could increase from 15 to 49 per cent. The unmet need for long-acting family planning methods is especially acute. Their use has not kept pace with that of short-acting methods, such as oral contraceptives and injectables. Data obtained from the Health and Health-related Indicators of Federal Ministry of Health (2007) show that the proportion of women using long-acting methods (0.4 per cent) is significantly lower than the proportion using short-acting methods (67.5 per cent) – which tend to be less effective and more expensive. |